Progress, but not success: why younger people are still stuck in aged care
Published on 7 April 2026

A new report from the Australian Institute of Health and Welfare reveals a system that has improved at the front door of aged care, but still struggles at the exit.
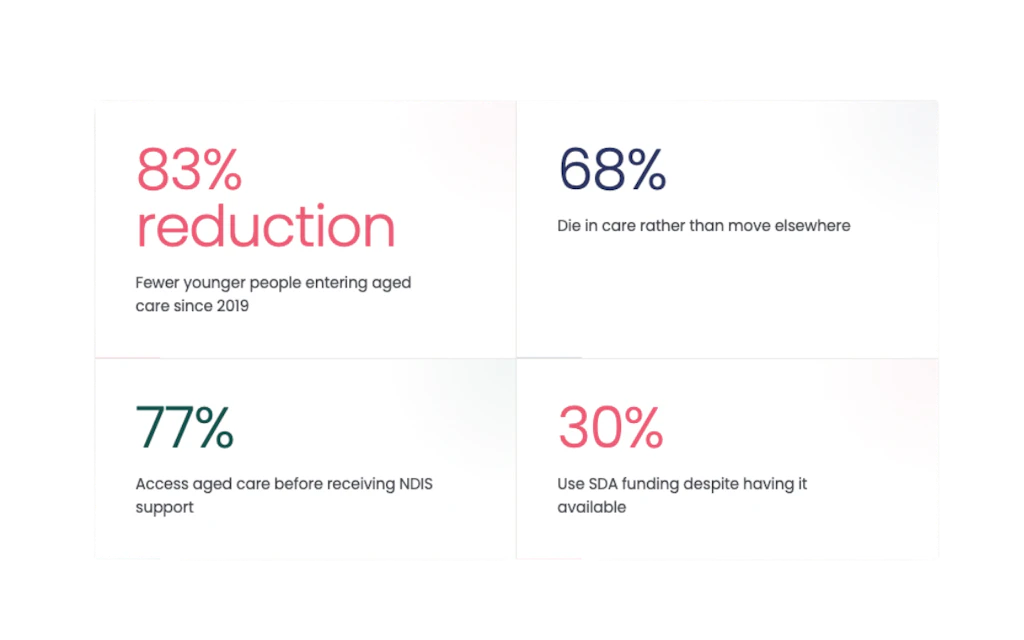
The number of younger people living in residential aged care has dropped sharply, down 83% from 5,216 in 2019 to 880 in 2025. On paper, that looks like reform working. In reality, it tells only half the story.
Because once younger people enter the system, leaving remains the exception, not the norm.
The real story isn’t who enters. It’s who never leaves
One of the more confronting findings is what happens after entry.
Around two-thirds of younger people who leave residential aged care don’t actually “leave” at all. They die there.
For those who do remain, many simply age out of the category, turning 65 and becoming part of the mainstream aged care population. In other words, the system isn’t resolving the issue. It’s absorbing it.
Even among NDIS participants, who are meant to have a pathway out, more than half either die in care or age out rather than transition to alternative housing.
So while policy has focused heavily on reducing admissions, the harder problem remains largely unsolved: enabling exits.
The NDIS is involved. But often too late
The NDIS is positioned as the primary pathway to more appropriate housing and support. But the timing tells a different story.
More than three in four younger people accessed aged care before they ever received an NDIS plan.
Even more telling, the majority only became NDIS participants after they had already entered residential aged care.
That flips the narrative. The NDIS isn’t consistently preventing entry. It’s intervening after the fact.
And by then, the system has already done what it does best: hold on.
Funding exists. Use of it does not
Here’s where things get quietly absurd.
One in five younger people in aged care who are on the NDIS have funding for Specialist Disability Accommodation. On paper, that should be a pathway out.
Yet fewer than one in three actually use that funding.
Not because they don’t need it. Because the housing often doesn’t exist.
This is the kind of detail that doesn’t make headlines but should. The system is approving solutions it can’t physically deliver.
The people missing from the conversation
Another detail that deserves more attention: not everyone in aged care has access to the NDIS.
Around one-third of younger people in residential aged care are not NDIS participants.
And this group looks very different.
They are:
- Older at entry
- More likely to have cancer or palliative care needs
- More likely to die in care
They sit in the gap between systems. Not quite eligible for disability support, but not well suited to aged care either.
Policy tends to orbit around the NDIS. This group sits just outside that gravitational pull.
A system designed for older people is still being used as a fallback
None of this should be surprising.
Aged care was never designed for people under 65. The report states this plainly.
And yet, it continues to function as the default when:
- housing is unavailable
- disability services are inaccessible
- hospital discharge needs a destination
It’s not always a failure of aged care. It’s often the absence of anything better.
The shift that hasn’t happened yet
There has been a clear policy focus on “diversion” avoiding entry into aged care. And it has worked.
Entries have dropped by more than 90% since 2019.
But diversion alone doesn’t solve the structural issue.
Because for the people already inside the system, the barriers are different:
- housing supply
- service coordination
- funding complexity
- and in some cases, clinical deterioration
The report hints at this, but doesn’t quite say it outright.
This is no longer a policy problem. It’s an infrastructure problem.
What providers should take from this
There’s a tendency to treat younger people in aged care as a legacy issue, something that will phase out over time.
This data suggests otherwise.
What providers are increasingly dealing with is a smaller, more complex cohort:
- higher clinical needs
- longer lengths of stay
- more behavioural and neurological conditions
- and often, no clear pathway out
NDIS participants, in particular, are entering younger and staying longer.
That changes the operational reality inside homes.
The uncomfortable conclusion
The sector has made real progress. Fewer younger people are entering aged care.
But for those who do, the system still struggles to offer a meaningful alternative.
Until housing, disability support, and health systems align in a way that actually enables exit, residential aged care will continue to carry a burden it was never designed for.
And quietly, behind the improvement headlines, that burden is becoming more complex, not less.