Residents say they’ve never been happier. The data tells a more complicated story.
Published on 29 April 2026

The latest national quality indicator data contains a headline worth celebrating: residential aged care residents are happier than they’ve ever been on record. But in the same dataset, hospitalisations are rising, and restrictive practices have quietly crept upward for four consecutive quarters.
The latest national quality indicator data contains a headline that the sector deserves to hear: residential aged care residents are reporting their highest ever levels of satisfaction and quality of life. But in the same dataset, quietly sitting beneath the good news, are two trends that complicate the picture considerably — and that are worth understanding before anyone gets too comfortable.
The Australian Institute of Health and Welfare’s latest quarterly report, covering October to December 2025, draws on data from 2,575 residential care homes across the country. It tracks 14 quality indicators spanning everything from pressure injuries and medication management to workforce turnover and consumer experience. And on most measures, the direction of travel is genuinely positive.
Pressure injuries are down. Unplanned weight loss is down. Antipsychotic medication use is down. Staff turnover is down. These are not trivial improvements — they represent thousands of individual Australians experiencing fewer episodes of preventable harm.
And the numbers residents are reporting about their own experience? Remarkable. 85.7% of residents rated their experience of their home as ‘good’ or ‘excellent’ — the highest figure ever recorded in this program. Quality of life ratings sit at 76.7%, also trending upward. In a sector that has endured years of public scrutiny and reputational damage, these numbers represent something meaningful.
So why does this report leave a nagging question rather than a clean sense of satisfaction?

Here is what the data actually shows. Over the past 11 quarters, residential aged care residents have consistently reported feeling better about their lives and their care. Consumer experience scores have risen from 79.7% to 85.7%. Quality of life ratings have climbed from 69.4% to 76.7%.
The paradox hiding in plain sight
Over that same period, the proportion of residents presenting to emergency departments has risen from 14.2% to 15.9%. The proportion experiencing an emergency department visit or hospital admission has remained persistently elevated, consistently above 19%.
Both lines are going up. At the same time.
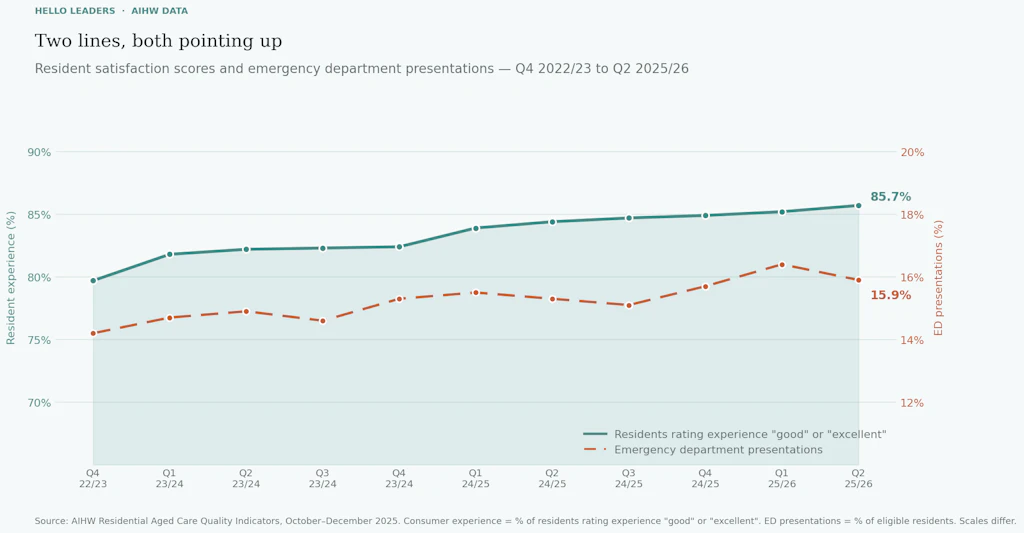
This is not presented here as a gotcha. The people who work in residential aged care have made genuine, measurable progress on many of the indicators that most directly affect residents’ physical safety and dignity. That progress is real and it matters.
But the coexistence of record satisfaction scores and rising hospitalisation rates asks a question that the sector should be willing to sit with: are we measuring resident experience, or resident safety? And when those two things diverge, which one tells us more about the quality of care being delivered?
The second signal no one is talking about
The hospitalisation trend has been rising for several years, and could reasonably be attributed to factors outside providers’ control — an ageing and increasingly complex resident cohort, pressure on GP access, changes in hospital admissions criteria. These are legitimate explanations.
The restrictive practices data is harder to explain away.
The report notes that there has been no statistically significant change in restrictive practices across the full 18-quarter trend period. But it flags — pointedly — that both restrictive practices indicators have shown a gradual increase across the most recent four quarters. The AIHW considers this notable enough to specifically call out when interpreting the data.
Four consecutive quarters of increase. Quietly. While everything else has been improving.

This matters because the timing is striking. The new Aged Care Act came into force on 1 November 2025 — the first month of the quarter covered by this report. One of its central commitments is a rights-based framework that treats restrictive practices as a last resort. The legislation is explicit. The expectations are clear.
And yet the last four quarters of data show a sector moving in the opposite direction on this specific measure.
That doesn’t mean the law isn’t working, or that providers are acting in bad faith. Restrictive practices data has always been complex to interpret — what counts, what gets documented, how different homes apply the definitions. There are legitimate clinical reasons why some uses may be appropriate and consented. The AIHW itself is careful to note these caveats.
But it does mean this is a trend worth watching carefully. And having a conversation about openly.

What the numbers can and can’t tell us
There’s a deeper question underneath all of this, and it’s one the sector would benefit from debating more honestly: what does “quality” actually mean in the context of residential aged care, and are the current quality indicators measuring it?
Consumer experience and quality of life surveys capture something genuinely important — the subjective sense of dignity, connection, and wellbeing that residents feel in their daily lives. That these scores are rising is meaningful. People feel seen, respected, and cared for.
But a resident can feel well cared for by staff who are kind and attentive, and still end up in an emergency department because a deteriorating condition wasn’t identified early enough, or because there wasn’t adequate clinical oversight available at the right moment.
Satisfaction and safety are not the same thing. And in a population that is older, more clinically complex, and increasingly arriving in residential care later than previous generations, the relationship between the two may be getting harder to sustain simultaneously.
The QI program has expanded significantly in recent years — from three indicators in 2019 to fourteen today, including new staffing measures for enrolled nurses, allied health professionals, and lifestyle officers introduced in April 2025. Each addition represents a genuine attempt to capture more of what matters. But every expansion also raises the question of whether the full picture is being seen.
What this quarter’s data actually asks of us
The honest read of this report is not that residential aged care is doing badly. It isn’t. Compared to where the sector was five years ago — in the midst of a Royal Commission that exposed systemic failures — the trajectory on most measures is genuinely encouraging.
The honest read is that the data is getting complex enough that simple narratives — whether triumphant or alarming — no longer serve the sector well. The people running residential homes across Australia need the real picture, not a curated one.
That means sitting with the discomfort of two things being simultaneously true: that staff are doing better work, in a more accountable environment, with more genuine care for the people they serve — and that more residents are ending up in hospital, and more are being subject to restrictive practices, than should be the case in a world where those commitments translated directly into outcomes.
The data deserves that honest conversation. So do the people living in residential aged care.
The AIHW Residential Aged Care Quality Indicators report for October to December 2025 was published 23 April 2026. Data covers 2,575 residential care homes. The full report is available at gen-agedcaredata.gov.au.